Don't get hurt in Hawaii
How a unique tax impacts the treatment of patients and pushes out primary care providers
Hawaii Island is short roughly 300 physicians. Statewide, that number is estimated to be well over 1,000.
In 2020 alone, 110 doctors retired in Hawaii County, 139 moved, and 120 worked shorter hours. But staffing shortages expand beyond doctors.
A report from the Healthcare Association of Hawaii found the overall need for healthcare professionals grew by 76% since 2019, listing 3,873 healthcare job openings in 2022 throughout the state.
This included a 116% job opening increase for registered nurses, a 162% increase for Medical Assistants, and a 110% increase for Social Workers.
In addition to a dwindling workforce, over one-third of the physicians in Hawaii are over the age of 60 and nearing retirement, the second highest percentage in the country.
The problem — outside of growing costs of living, rural access, and low Medicare, Medicaid and TRICARE reimbursement rates — is a unique General Excise Tax for the state of Hawaii, known as the GET.

In 1931, Hawaii established a traditional retail sales tax, which was repealed and replaced with an overall tax on businesses for all transactions including medical care, food, and medicine. What started as a 1.5% tax to supplement the state’s budget has grown into a 4.712% tax for Hawaii County as of 2020.
The rising cost has not only impacted patients, but private practice providers.
“We’ve had a shortage of healthcare providers for as long as I can remember,” said Dr. Scott Grosskreutz, a radiologist leading the Hawaii Physician Shortage Crisis Task Force. Grosskreutz has been working with the nonprofit Grassroot Institute to push for statewide GET reform.
“On the Big Island, we had a 53% shortage of doctors, meaning we had less than half of what we were projected to need, and one of the things we can do here to really help is pass GET reform,” he said. “We’ve had a number of candidates from both parties that are supportive of the idea.”
In 2020, State Senate Bill 2542 proposed exempting medical services from the GET, which would have placed providers on an equal playing field as hospitals and other nonprofits that are currently exempt.
The bill noted these forms of taxation already “disproportionately and adversely affect low-income and middle class families struggling to cope with the state’s high cost of living.” In certain cases, the GET tax can be passed on to patients.
The GET charge to patients is often the easiest way for a provider to recover their expenses, but under consumer protection laws, the amount that is visibly passed on and represented to be the GET cannot exceed the actual tax due on the transaction.
“Only Hawaii and New Mexico will charge a patient a tax if you get sick or injured,” said Grosskreutz. “It’s hard to describe that as anything other than, in my opinion, unethical.”
While the bill made its way through the Senate, passing 25-0, it failed to get through the House, with Grosskreutz citing the chaos of the pandemic as a main factor behind the inaction.
“But of course, lawmakers also see (reform) as a loss to them, because that’s from their budget,” said Joe Kent, executive vice president for the Grassroot Institute.
While efforts to reintroduce the bill in 2021 took place, Grosskreutz said he heard concerns from lawmakers regarding “budget deficiency.”
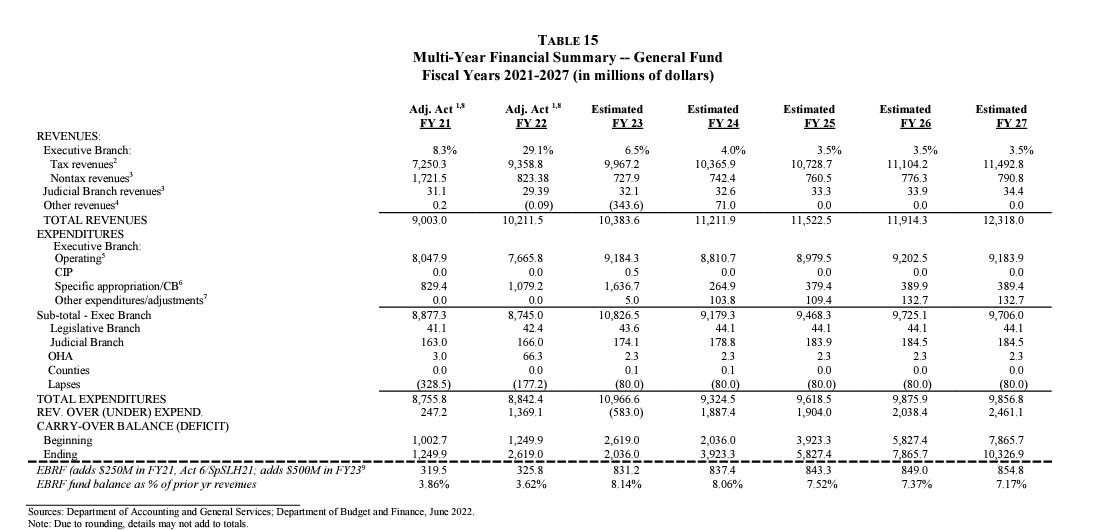
According to a 2021 report from the Hawaii Physician Shortage Crisis Task Force, the GET generates more than half of Hawaii’s tax revenue, but Grassroot Institute estimates, and a recent bond sale confirms, that the 2023 fiscal year budget had a surplus of nearly $4 billion.
“That surplus is projected to grow to $10 billion by (Fiscal Year) 2027,” Kent said. “Keep in mind that these are abnormally high surpluses.”
Former governor David Ige warned during an exit interview with the Honolulu Star-Advertiser that potential changes to the GET can result in negative consequences.
“It’s easy to say as a candidate that (reform) is a good thing to do,” Ige said. “But I think those in the Legislature also realize that as you chip away at the General Excise Tax, where does it end? There’s always a lot of things people think we shouldn’t tax, and as you begin to exempt them, then the excise tax becomes less and less efficient, and you end up raising taxes someplace else.”
But there’s a caveat. A study conducted by Grassroot Institute estimated GET reform on medical care could save private practice doctors roughly $222 million a year, and another report from the American Medical Association found that physicians, on average, generate roughly $3 million in economic activity via renting space, hiring local staff, acquiring accountants and using other community resources.
With a shortage of roughly 1,000 physicians statewide, Grassroot Institute estimates increasing the workforce at this scale could bring in an additional $3 billion to the state’s economy, a significant increase from the $200 million the GET on medical currently generates.
“As the number of people in private practice get pushed out — it’s already below 50% for the state — but as they have to quit or retire, and no one comes to take them over, you’ll have fewer and fewer people in private practice being taxed,” Grosskreutz said. “In the long run, maybe in as little as three-to-five years, there will be little revenue from taxing healthcare because you won’t have any people in private practice left to tax.”
To advocate for change, the institute launched a petition, pushing for GET exemption on medical care. So far, that petition has earned only 1,150 signatures. But one key supporter might hold the power.
Recently-elected governor Josh Green, a former physician on the Big Island, spoke publicly during his inauguration in favor of addressing GET reform for food and medicine. But it remains unclear if medicine and medical services fall into the same category.
“The poorest families are hit the worst, and those who are struggling to survive from paycheck to paycheck really can’t afford that tax,” said Green, a Democrat, to loud applause.
Green is hoping the loss of revenue could be supplemented by a proposed “climate impact fee,” where the state would charge $50 to all incoming tourists 12 and older. With between 7-8 million annual visitors, Green estimates the state could generate nearly $350 million per year from the fee.
“A lot of times, you’ve got private insurance, where it’s the patient that pays the tax because the healthcare provider or hospital passes it on,” Grosskreutz said. “And if you’re already staggering under large medical bills, because you have cancer or need heart surgery, the last thing you can afford to do is pay the state tens of thousands of extra dollars in GET taxation.”
Dr. John Wade of the Hawaii Physician Shortage Crisis Task Force called the tax “a private practice killer” in a 2021 report.
“The Legislature has been reluctant to give the relief to the solo and small practice providers, although the hospitals don’t pay it and neither do the federally qualified health centers,” said Lisa Rantz, executive director of the Hilo Medical Center Foundation. “The big institutions say if they had to pay it, it would put them out of business…By straddling it on the solo and small practice guys whose margin is so thin, it doesn’t make a whole lot of sense. If they didn’t have to pay that, that could potentially lead to more employees, which could generate more income.”
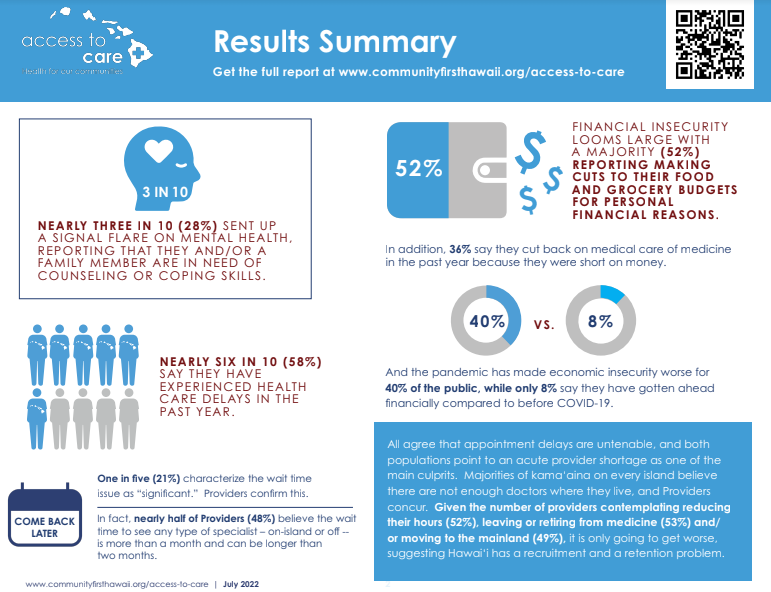
The shortage of providers has been felt by the public, with a recent Access to Care survey from Community First Hawaii reporting 82% of residents on Hawaii Island thought there were not enough providers in general. Another 58% said they experienced healthcare delays as a result of the shortage.
A lack of providers can also lead to other complications for patients, including longer wait times for cancer screenings and ultimately the delay of lifesaving treatment.
In October, Hawaii Radiologic Associates experienced a ransomware cyberattack, shutting down screening services as well as online and phone servers at all of its Hawaii Island locations. As the only radiologic imaging center on the island, patients were forced to reschedule or delay appointments, seek services at the overwhelmed Hilo Medical Center and Kona Community Hospital, or simply wait it out, putting off potentially life-saving screenings.
Francine Souza was attempting to schedule an appointment with HRA for Oct. 28 for a bone density scan and mammogram. But she was greeted with a voice message, letting her know appointments would be pushed back until the week of Nov. 13 due to the cyberattack.
“This is putting lots and lots of women at high risk,” said Souza. “Can you imagine all those backed up appointments? Can you imagine all those misses?”
Hawaii Island is already experiencing a 50% shortage of radiologists, according to one University of Hawaii annual report.
Healthcare providers throughout the community commented on the incident and the cracks it revealed in the current system.
“They have been the sole source of outpatient radiology services in our community all the time I’ve been practicing here,” said Big Island Docs President and local healthcare provider Lynda Dolan. “If they weren’t here, I really don’t know what we would do.”
“We’ve been sending all our patients to Hilo Medical Center,” added Dr. Pradeepta Chowdhury during the closure. “They’re getting overwhelmed with all the community referrals. But that’s the only option left to us.”
But Hilo Medical Center is suffering from both staffing and bed shortages as well.
“It’s the fact that we’re so full. We cannot care for all of our patients,” Hilo Medical Center Intensive Care Unit Nurse Ashley Mae told Hawaii News Now in 2022, adding the hospital had 75 full-time positions that still need to be filled.
The Hawaii State Rural Health Association estimated that wait times can be more than six months for certain patients seeking treatment.
"And even for cancer patients, which is unheard of, because that can be the difference between life and death," Lisa Rantz, president for the Hawaii State Rural Health Association, told KITV in 2022. "It's frightening to look at the shortages that we're experiencing across the board."
Add to these strenuous circumstances the data from the Access to Care survey, which reported 49% of healthcare providers considered moving to the mainland, 53% considered retiring or leaving medicine, and 52% considered reducing their hours.
Reimbursement rates associated with Medicare, Medicaid and TRICARE patients are also making it difficult for doctors and their practices to stay in Hawaii.
“The economic reality is the cost of providing medical care in Hawaii is often higher than what those reimbursements are,” said Grosskreutz. “When you have these very high costs in the state of Hawaii, and then very low reimbursements, and then on top of that you have the state taxing you on your patients care, it basically guarantees that if you’re breaking even providing services, you’re going to lose money, and if you were losing money before, you’re going to lose even more money now.”
The reimbursements offer funds to doctors and health facilities providing medical services to Medicare, Medicaid and TRICARE patients, and with 50% of patients requiring the reimbursements, Grosskreutz believes there’s little incentive for providers to stay on the islands.
“One of the problems that we have is this very, very low rate of medicare reimbursement in the state of Hawaii,” said Grosskreutz, who noted Medicare and Medicaid are about to cut reimbursements again by 8.5% in 2023.
When those reimbursements are cut, physicians opt to limit the number of federally covered patients they treat in order to meet their financial bottom lines and keep their practices afloat. As a result, patients lose access to lifesaving services.
A 2020 survey from the Medical Group Management Association found 92% of practices nationwide reported Medicare reimbursements did not cover the cost of caring for patients, a significant challenge for Hawaii, which has one of the lowest Medicare reimbursement rates in the nation.
“Our healthcare workers in general are understaffed, they’re overworked, and they’re aging out,” said Grosskreutz, who despite all this, remains hopeful. “It’s going to really take the general public and the community to lobby for these things to get them passed this session.”
The takeaway, whether a visitor or a resident, is to just not get hurt in Hawaii.